South Florida Teacher Infected With MRSA “Superbug”

Tresca Jenkins, a third grade teacher at Sunset Elementary in South Florida, is in quarantine with the superbug on Wednesday.
Attorney Mitchell J. Panter was recently interviewed about his client’s current conditions. Click here to watch the video from NBC 6 News.
Methicillin-resistant Staphylococcus aureus (MRSA), also known as the “Superbug”, is a biological agent responsible for difficult-to-treat infections in humans. MRSA is a variation of the common bacteria, Staphylococcus aureus. It has evolved the ability to survive treatment with beta-lactam antibiotics, including penicillin and methicillin.
Signs & Symptoms of MSRA:
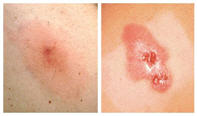 Staph infections, including MRSA, generally start as small red bumps that resemble pimples, boils or spider bites. These can quickly turn into deep, painful abscesses that require surgical draining. Sometimes the bacteria remain confined to the skin. But they can also burrow deep into the body, causing potentially life-threatening infections in bones, joints, surgical wounds, the bloodstream, heart valves and lungs.
Staph infections, including MRSA, generally start as small red bumps that resemble pimples, boils or spider bites. These can quickly turn into deep, painful abscesses that require surgical draining. Sometimes the bacteria remain confined to the skin. But they can also burrow deep into the body, causing potentially life-threatening infections in bones, joints, surgical wounds, the bloodstream, heart valves and lungs.
Risk Factors:
Because hospital and community strains of MRSA generally occur in different settings, the risk factors for the two strains differ.
Risk factors for hospital-acquired (HA) MRSA include:
- A current or recent hospitalization. MRSA remains a concern in hospitals, where it can attack those most vulnerable – older adults and people with weakened immune systems, burns, surgical wounds or serious underlying health problems. A 2007 report from the Association for Professionals in Infection Control and Epidemiology estimates that 1.2 million hospital patients are infected with MRSA each year in the United States. They also estimate another 423,000 are colonized with it.
- Residing in a long-term care facility. MRSA is far more prevalent in these facilities than it is in hospitals. Carriers of MRSA have the ability to spread it, even if they’re not sick themselves.
- Invasive devices. People who are on dialysis, are catheterized, or have feeding tubes or other invasive devices are at higher risk.
- Recent antibiotic use. Treatment with fluoroquinolones (ciprofloxacin, ofloxacin or levofloxacin) or cephalosporin antibiotics can increase the risk of HA-MRSA.
These are the main risk factors for community-acquired (CA) MRSA:
- Young age. CA-MRSA can be particularly dangerous in children. Often entering the body through a cut or scrape, MRSA can quickly cause a wide spread infection. Children may be susceptible because their immune systems aren’t fully developed or they don’t yet have antibodies to common germs. Children and young adults are also much more likely to develop dangerous forms of pneumonia than older people are.
- Participating in contact sports. CA-MRSA has crept into both amateur and professional sports teams. The bacteria spread easily through cuts and abrasions and skin-to-skin contact.
- Sharing towels or athletic equipment. Although few outbreaks have been reported in public gyms, CA-MRSA has spread among athletes sharing razors, towels, uniforms or equipment.
- Having a weakened immune system. People with weakened immune systems, including those living with HIV/AIDS, are more likely to have severe CA-MRSA infections.
- Living in crowded or unsanitary conditions. Outbreaks of CA-MRSA have occurred in military training camps and in American and European prisons.
- Association with health care workers. People who are in close contact with health care workers are at increased risk of serious staph infections.
When to Seek Medical Advice:
Keep an eye on minor skin problems – pimples, insect bites, cuts and scrapes – especially in children. If wounds become infected, see your doctor. Ask to have any skin infection tested for MRSA before starting antibiotic therapy. Drugs that treat ordinary staph aren’t effective against MRSA, and their use could lead to serious illness and more resistant bacteria.
